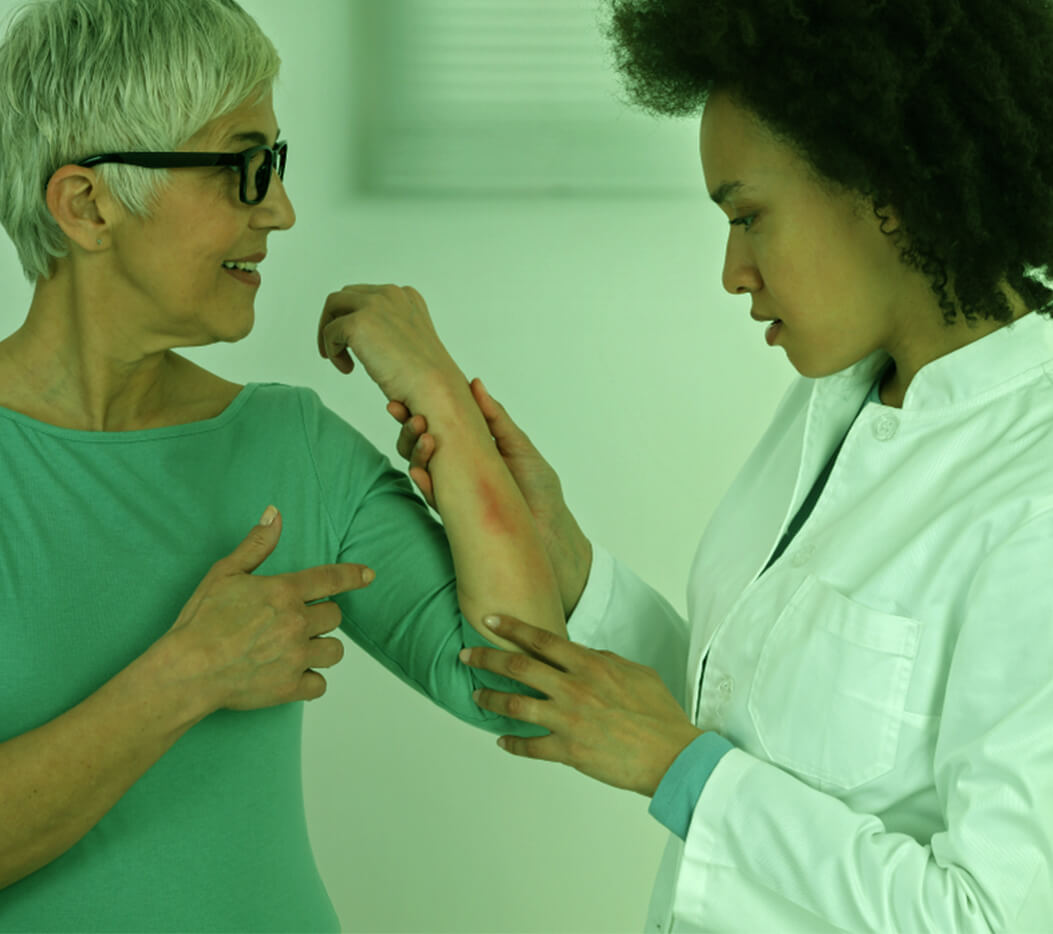
Are You Allergic to Your Clothes ?
When certain physical or chemical agents come into direct contact with the skin, they might trigger an allergic reaction, causing the skin to become inflamed, red or itchy. This response is known as contact dermatitis.
There are two distinct types of contact dermatitis :
1] Irritant dermatitis :
This is a direct response of the skin cells to a causative agent. As soon as the skin is exposed to the irritant, the epidermal cells release mediators, which initiate and regulate skin inflammation. Although the intensity of the reaction depends heavily on the duration of exposure and the chemical components of the irritant, it is also influenced by existing skin conditions and disorders, and environmental factors such as humidity, temperature, etc.
Physical irritants include friction and grazing.
Chemical irritants include hand soaps, detergents, etc.
2] Allergic contact dermatitis :
When the skin is exposed repeatedly to an allergen, it gradually becomes sensitised to the allergen, leading to inflammation and irritation. The causative agent first penetrates the outermost layer of the skin, after which it merges with skin proteins, producing an immune response. The skin may take 5 to 21 days to grow sensitised to the allergen. Common causes of allergic contact dermatitis include chromium, neomycin, nickel, balsam of Peru and cobalt. Allergens are often also present in jewellery.
There are certain factors which predispose individuals to developing AECD:
-
Genetic make-up, the consumption of certain drugs and certain existing diseases may make an individual more susceptible to AECD.
-
If the patient’s skin is prone to irritation and inflammation, or is already diseased, he/she might be more prone to AECD.
-
Occupation, environment and geographical location are responsible for the chemicals or substances that the individual is exposed to.
-
Psychological factors such as stress may exacerbate symptoms of contact dermatitis. Certain hormonal imbalances may also encourage the development of dermatitis.
Occupational exposure :
You may be exposed to certain irritants at the workplace, which may either cause an immediate allergic reaction, or sensitise the skin over a period of time. Agricultural workers, factory employees, cooks, mechanics, healthcare workers, cleaners, etc. are constantly exposed to potential allergens and irritants. The hands are one of the most common sites for contact dermatitis. Common irritants include paints, solvents, oils and detergents, while metals, epoxy resins, rubber, etc. are potential allergens.
Allergies to medicines and medical equipment :
Some creams contain preservatives, such as propylene and butylene glycols; parabens; benzyl alcohol, sodium metabisulphate; lanolin, etc.
Topical corticosteroids can also trigger AECD.
Latex-based medical equipment such as gloves, catheters, intubation tubes, etc., when exposed to over a long period of time, may lead to the development of AECD.
Photocontact dermatitis :
Certain substances, either when consumed or applied directly to the skin, may become irritants (phototoxic) or allergens (photoallergenic) when exposed to sunlight.
Phototoxic dermatitis is an immediate response, and occurs when the substance becomes an irritant in the presence of sunlight. It mostly develops during or after the first exposure.
Photoallergenic dermatitis develops over a period of time. The skin (mostly of the face and the hands) experiences inflammation as a delayed response to exposure.
Possible topical agents include: detergents, bleaching powders, soaps, cosmetics and lotions, ointments and perfumes.
Possible systemic agents include: antibiotics, anti-bacterial medications, diuretics and antifungal medications.
Symptoms :
Although the clinical presentation of contact dermatitis may vary depending on whether it is irritant or allergic in nature, common symptoms include redness, itching, rashes and inflammation. The skin may appear scaly, with well-defined borders.
A more detailed description of the symptoms is provided in the table below.
| Category |
Irritant Contact Dermatitis |
Allergic Contact Dermatitis |
| Location |
Often the hands |
Areas that are relatively more exposed, eg. hands and face |
| Common symptoms |
Burning sensation, itchiness (pruritus), pain or discomfort |
Itchiness is the main symptom |
| External appearance |
Cracked, dry skin |
Fluid-filled sacs or blisters on the surface of the skin. |
| Demarcations |
Borders less apparent |
Well-defined borders. |
Diagnosis
A full history of the patient’s occupation, pastimes and topical or systemic medication should ideally be taken into account when diagnosing contact dermatitis.
Patch testing is considered to be most effective. Patches contain small amounts of chemicals, metals, medicinal substances, rubber, dyes, and a variety of other additives to which the patient may potentially have developed an allergy. These substances are present in a diluted form. The patches are then applied to the patient’s back for 48-72 hours, where a localised allergic reaction may develop. This helps determine the causative agent.
Treatment
-
Avoidance. It is recommended that soaps, fragrances and detergents be avoided completely, and the possibility of friction minimised. If the cause of contact dermatitis is occupational, the patient should ideally wear some form of protective equipment, such as gloves.
-
Antihistamines may help soothe the itchiness. Hydroxyzine and cetirizine are highly recommended.
-
Certain ointments, namely tacrolimus, help suppress calcineurin, a protein phosphate responsible for activating T-cells and causing a reaction.
-
Emollients and palliatives rehydrate the skin by creating an oily coating on its surface, which helps trap moisture.
-
Systemic steroids, which are only used for serious reactions.
-
Inflammation can be reduced by administering high-potency topical corticosteroids. These, however, should not be applied to areas where the skin is particularly thin, as they put the epidermis and dermis at risk of degradation.